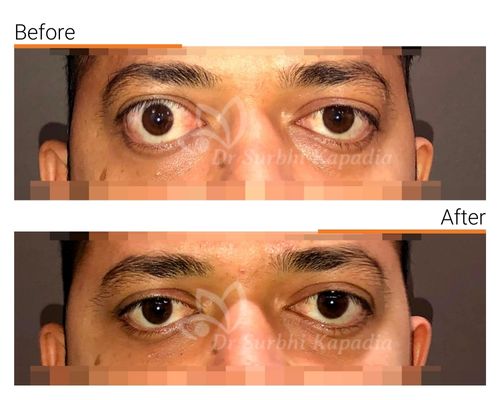
What is Thyroid Eye Disease?
Thyroid Eye Disease, often abbreviated as TED, is a condition often seen in patients with thyroid abnormalities, leading to changes in the eyelids and orbital region (the bony cavity housing the eyes). The disease often results in the retraction of the upper and lower eyelids, causing the eyes to appear more prominent, a condition also known as proptosis.
Thyroid Eye Disease is primarily caused by an autoimmune response, resulting in the deposition of proteins and swelling of the eye muscles. This causes the eye to swell within its bony socket, known as the orbit.
The symptoms of Thyroid Eye Disease can include swollen eyes, redness, protrusion of the eyes (proptosis), double vision, watering, pain, dimness of vision, and changes in the position of the eyelid.
Treatment for Thyroid Eye Disease can involve several strategies. Lid surgery can be effective for cases of minimal proptosis, while more severe cases may require orbital decompression surgery, a procedure which creates space in the bony orbit behind the eye, allowing the protruding eyeball to be pushed back. Some severe cases may require both of these surgeries in two stages for optimal results.
The active phase of Thyroid Eye Disease typically lasts from 6 to 12 months after onset. Following this, the disease typically enters an inactive stage. However, a second active phase may occur in some individuals.
Nighttime dryness and irritation, known as nocturnal lagophthalmos, are common in patients with Thyroid Eye Disease. Good lubricating eye gels, used under the supervision of an ophthalmologist, along with protective glasses can be helpful.
Delaying treatment, continuing to smoke, and uncontrolled thyroid levels can lead to the worsening of Thyroid Eye Disease. Following your eye doctor’s instructions during the active phase of the disease is crucial.
While the active phase of the disease is generally well-managed by medical treatment, the inactive disease often requires surgical management by expert ophthalmic plastic surgeons. The Department of Ophthalmology & Ophthalmic Plastic Surgery at Aadicura Superspeciality Hospital offers comprehensive solutions for medical management, orbital decompression, and cosmetic surgery for Thyroid Eye Disease.
Controlling thyroid levels through medications, avoiding smoking, and improving your lifestyle can help manage Thyroid Eye Disease. Regular checkups and consultations with your eye doctor are crucial in controlling the disease and improving your condition.
Yes, people with Thyroid Eye Disease can close their eyes. However, they might experience difficulty fully closing their eyes due to the swelling and retraction of the eyelids, which can lead to dryness and exposure symptoms. This condition is known as lagophthalmos.
The eye bulging, also known as proptosis, is primarily caused by the swelling and inflammation of the muscles and tissues located behind the eye. This inflammation can push the eyeball forward, leading to the characteristic eye bulging seen in TED.
Thyroid Eye Disease is usually diagnosed based on the patient’s clinical symptoms and physical examination of the eyes and eyelids. Additional tests, such as a blood test to measure thyroid hormone levels and imaging studies like a CT scan or MRI, can help confirm the diagnosis.
Thyroid Eye Disease is an autoimmune condition, meaning it’s caused by the immune system mistakenly attacking the body’s own tissues. Removing the thyroid can help manage the hormonal imbalances that contribute to TED, but it won’t cure the eye disease itself. Treatment of the eye condition will still be needed.
Thyroid Eye Disease is detected through a comprehensive eye examination that includes a patient’s medical history and several visual tests. Your doctor will check for common signs of TED, like eyelid retraction and eye bulging. Imaging tests, like a CT scan or MRI, can help confirm the diagnosis.
Treatment for Thyroid Eye Disease often involves managing symptoms and protecting the eye. This can include the use of artificial tears for dryness, wearing sunglasses to protect from light sensitivity, and sleeping with the head elevated to reduce swelling. More severe cases may require surgical intervention, such as orbital decompression surgery or eyelid surgery. Medical treatments such as corticosteroids or newer biological therapies may also be used to manage inflammation.
Ophthalmic Plastics
Orbit and Ocular Oncology
Trauma
Non-surgical Cosmetic Procedures
Surgical Cosmetic Procedures